Vision Problems
When it comes to eye health care, it helps if you have a clear understanding of common vision problems, including their causes and solutions. Causes of blurred vision typically fall into two main categories.
1. Eye Focusing issues
The misfocusing of light in the eye, also known as refractive errors, is the most common cause of blurred vision. This is usually due to the eye being slightly too long, too short or irregularly shaped. Our optometrists can diagnose this and help you see clearly again with prescription glasses or contact lenses.

2. EYE HEALTH CONDITIONS
To see your best your eyes need to be healthy. Cataracts, glaucoma, macular degeneration and dry eye are some common conditions that cause blurred or reduced vision. Some serious eye conditions, if not detected and taken care of promptly, can cause permanent loss of vision.
Eye Focusing Issues
Refractive errors arise from the misfocusing of light in the eye. Below are the four most common causes of refractive errors — all of which can be corrected by our optometrist with prescription glasses or contact lenses, so you can see clearly again.
Myopia
also called "short-sightedness" or "near-sightedness"
近视

Myopia is commonly caused by the eye growing slightly too long, so light is misfocused in front of the retina. The longer the eyeball, the greater the degree of myopia. Myopia typically begins in childhood and worsens in adolescence as the eye grows.
A person with myopia can see close objects clearly, while objects in the distance will appear blurry. A child with myopia may find it hard to see the whiteboard at school, while an adult may have trouble seeing signs when driving, or recognising faces from a distance.
Myopia development is influenced by both genetics and environmental factors. Having one or both parents with myopia, and spending a lot of time indoors, reading too close to your face, doing school work, or using a tablet and computer all increase the risk of developing myopia.
Myopia is the most common vision problem in children and young adults and it poses the greatest risks for the long-term health of the eyes. However, with proper eye health care, such as our Myopia Control Solutions, your myopia can be corrected or treated.
Hyperopia
also called "farsightedness" or "long-sightedness"

Hyperopia occurs when the eye is too short. Low amounts of hyperopia is common in kids and usually isn't a major eye health care problem as children's eyes can adjust focus to compensate. However, some children may experience discomfort and headaches from the constant focusing.
A far-sighted person can see things at a distance clearer than if they are nearby. They need to work their eyes harder to focus up close, and to maintain that focus. Over time this causes the eye muscles to strain, often leading to headaches, sore eyes and tiredness.
Symptoms of hyperopia may be relieved by solutions such as glasses, eye exercises or taking more breaks from close-up work. In children, a high degree of uncorrected hyperopia, particularly if only in one eye, can cause eye misalignment (strabismus) and lazy eye (amblyopia).
Astigmatism
sometimes also called "cylinder" or "football-shaped eye"

Astigmatism is an irregularity or imperfection of the front surface of the eye. Instead of being perfectly round, the eye is oval-shaped. Astigmatism is very common - around half of people with glasses have some amount of astigmatism in their glasses prescription.
People with astigmatism can have blurred vision both far away and up close. Some describe the blur as an overlapping shadow, which is very uncomfortable for the visual system. When not properly cared for, astigmatism can often cause health problems such as headaches and eye strain.
Astigmatism can occur alone or in combination with nearsightedness and farsightedness. Most types and degrees of astigmatism can be corrected fully by glasses and contact lenses. Contact lenses for astigmatism are often referred to as 'toric lenses'.
Presbyopia
the loss of focusing flexibility with age
老花眼

As we age, our eyes gradually lose flexibility like the rest of our bodies. The lens inside our eyes becomes less elastic and less able to quickly adjust focus. Changing our focus from distance to near, and vice versa, becomes slower. Reading and detailed close-up work becomes increasingly harder.
People with normal distance vision will start to hold their book further away to read more comfortably. Those who are naturally near-sighted may find reading up close easier without their long-distance glasses, and farsighted people will find reading up close very difficult and uncomfortable.
Presbyopia tends to occur at around age 45, but it could be earlier for some and later for others. Prescription reading glasses will help. For those who are already wearing glasses for distance, multifocal or bifocal lenses may be the best eye health care solution to correct both the long and short distances in a single pair of glasses.
other eye conditions
Eye Health Conditions
Below are common eye health conditions and diseases which can cause blurred vision, and in some cases lead to severe loss of vision.
Our optometrists are trained to detect, diagnose and manage these eye conditions, as well as other eye health issues. Where necessary, we can also provide referrals to ophthalmologists (eye specialists) for further examination and management. If in doubt, book an appointment with us today to learn more about our eye care solutions.
Cataract
白内障
A cataract is a clouding or yellowing of the eye's natural crystalline lens. Most often occurring with age, cataracts usually develop slowly, gradually making vision more blurry, like looking through a foggy window. It also causes significant glare.
Glaucoma
青光眼
Glaucoma occurs when the optic nerve is damaged by a build-up of pressure inside the eye. Over time it causes irreversible loss of peripheral (side) vision. Glaucoma runs in families and a more aggressive type is a common eye health care problem among people of Asian descent.
Macular Degeneration
黄斑病变
Macular degeneration (AMD) is a progressive disease of a critical central area of the retina. It causes painless, permanent loss and distortion of central vision. In advanced cases it can affect a person's ability to drive, read, see fine detail and recognise faces.
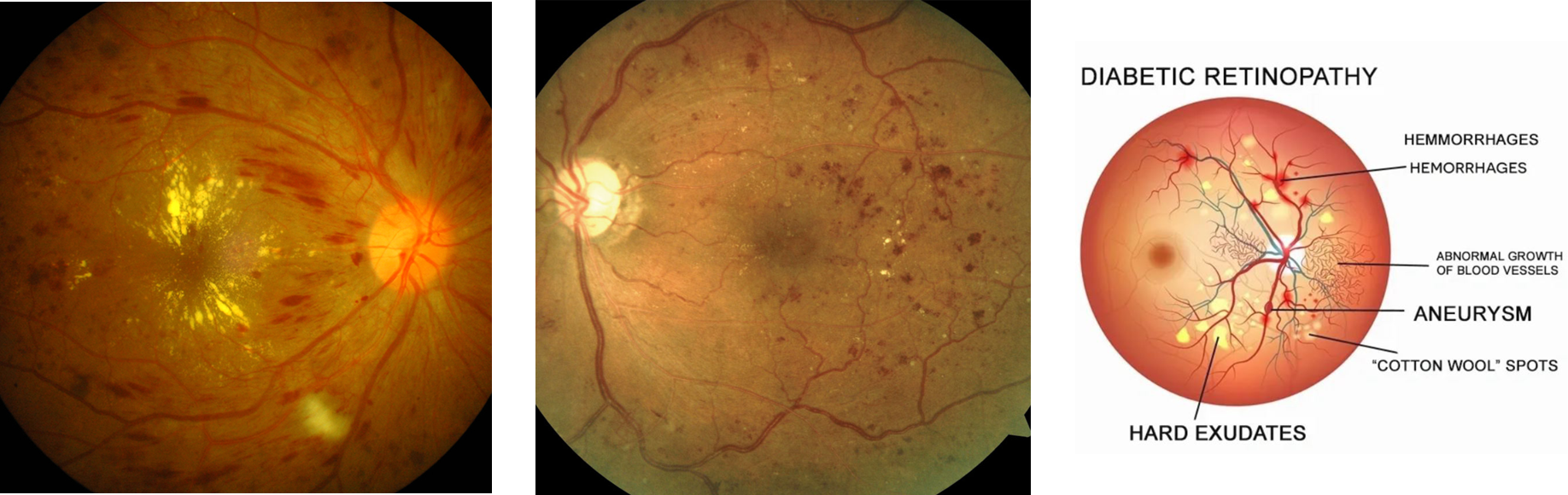
Diabetic Retinopathy
糖尿病性视网膜病变
Diabetes causes blood vessel changes throughout the body, and in the eye it can cause leaky new vessels, bleeding, vision loss and serious complications. An optometrist can sometimes detect diabetes before a patient is aware they have the condition.
Floaters
飞蚊症
Floaters are small protein fibres from the gel-like substance called the vitreous at the back of the eye. They appear as black or grey spots, strands or cobwebs. Large floaters can cause blurred vision. If new floaters occur with flashes of light, have your eyes checked immediately.
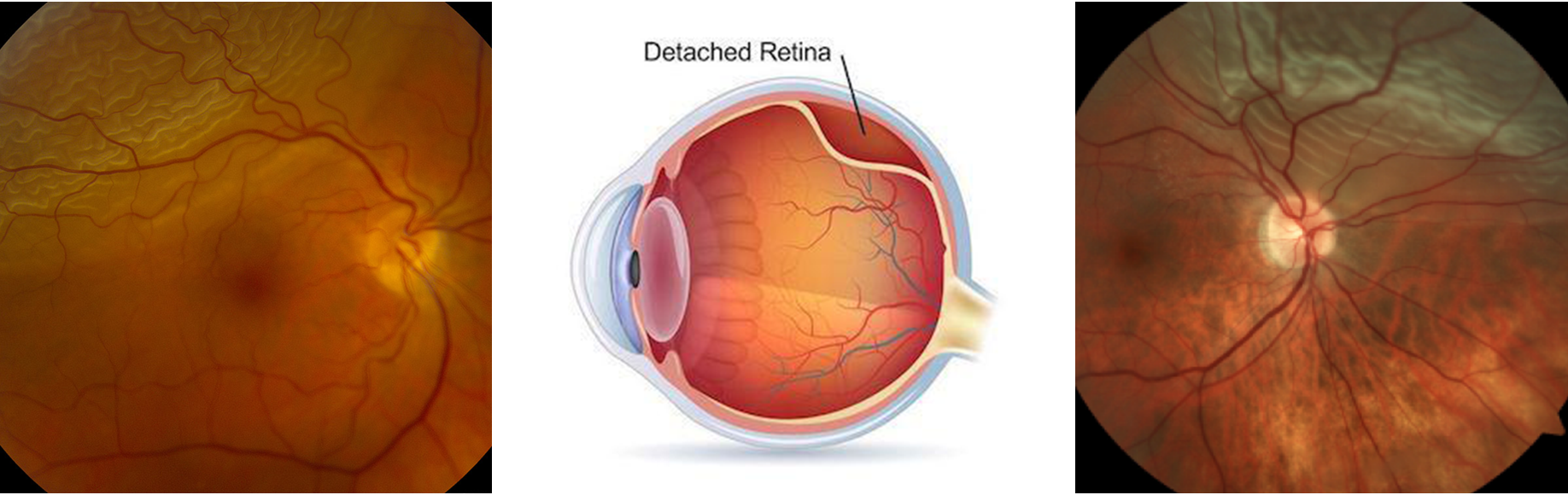
Retinal Lesions
视网膜病变
Retinal lesions can be serious and lead to permanent vision loss. Retinal detachment, where the retina peels away from the back of the eye, can occur with trauma or age, and people with higher degrees and short-sightedness are at much higher risk.
Eye Infection
眼部感染
Eye infections are common, especially in kids. Bacterial conjunctivitis is particularly contagious. Contact lens wearers are also at a higher risk of developing infections. Our optometrists are qualified to identify and diagnose these conditions and provide appropriate care for your eye health.
Dry Eye
干眼症
Dry eye is a common, sometimes chronic condition, that can occur at any age. It may cause blurred vision that comes and goes. Other symptoms include irritation, redness, stinging or burning sensation, mucus around the eyes, and itchy, tired or watery eyes.
Pterygium
翼状胬肉
A pterygium is a slow, benign growth of the eye's outer membrane onto the cornea, forming a triangular lump of tissue. In more advanced cases it can interfere with vision. It is common in Singapore and is associated with exposure to the sun and UV light.
It is important to address eye health conditions before they progress and lead to more severe problems. Our optometrists are fully qualified to provide eye care for the conditions listed above. Contact us today to find out more.